GHA’s IMPACT™ Study* found that growth in cross-border care is not constrained by demand. It is constrained by trust. The data also shows that trust is not produced by clinical quality alone. It is shaped by how care is communicated, coordinated, and experienced across the full patient journey.
One finding is particularly consequential for accreditation. A significant proportion of patients receive care at accredited facilities, yet many are unaware of that accreditation status. When accreditation is not visible, its trust advantage is lost. When it is visible, patient confidence, satisfaction, and likelihood to recommend increase significantly.
This gap between accreditation achievement and patient awareness is not simply a communication issue. It is a structural issue with direct implications for how accreditation creates value and how standards must evolve.
Its significance becomes clearer when considering who today’s cross-border patients actually are. International travel for treatment is often imagined as a service for the wealthy. The data show otherwise. Many cross-border patients today are middle-income workers traveling under employer benefit programs, public payers contracting capacity abroad, and regional populations whose nearest viable specialist sits across a border. International patient services are no longer a parallel economy. They are part of how delivery systems manage capacity, workforce, and access for the populations they serve.
Within this context, accreditation is also being redefined. Traditional models have played a critical role in advancing clinical quality and patient safety. However, as care delivery becomes more interconnected and patient journeys extend across systems, geographies, and timeframes, the question is no longer only whether care meets standards at a single point. It is whether the entire experience can be delivered in a way that is coordinated, transparent, and trusted.
It is within this context that Global Healthcare Accreditation’s forthcoming Accreditation 6.0 standards have been developed. Rather than representing an incremental update, Version 6.0 responds directly to the gap between validated quality and experienced trust. It reflects a broader shift in how quality is defined in global healthcare, with greater emphasis on transparency, system coordination, and the ability of organizations to make quality visible and meaningful to patients, not only measurable internally.
Understanding the Shift: Benchmarking as a Foundation
The development of Accreditation 6.0 is closely tied to the findings of the 2026 Global Medical Travel Benchmarking Report, which brings together insights from accreditation activities, cross-border patient interviews, high-performing program reviews, and global data sources. Its purpose is to move beyond comparison and toward clarity on how expectations are changing, where performance gaps persist, and what defines readiness in an increasingly competitive global environment.
Across regions and healthcare systems, a consistent pattern emerges. Organizations are not struggling to deliver high-quality clinical care. Rather, they are encountering challenges in delivering that care as part of a seamless and accountable patient journey. Breakdowns occur in the transitions between stages of care, in communication across teams, and in the continuity of engagement once the patient leaves the clinical setting. An illustrative example comes from a GHA accredited hospital in Southeast Asia, which addressed these gaps by replacing a traditional CRM with a comprehensive digital patient journey platform. As a result, Service Level Agreement (SLA) compliance improved dramatically from 40 percent to 92 percent, while documentation errors were significantly reduced, demonstrating how integrated journey management can materially improve operational reliability and continuity of care.
This shift has important implications. What once differentiated leading programs is rapidly becoming the expected baseline. The ability to manage care across the full patient journey, to align governance and decision-making, and to ensure continuity through digital and operational systems is no longer optional. It is increasingly how quality is judged.
Measuring What Matters: Insights from the IMPACT™ Study
While benchmarking reveals how organizations operate, the IMPACT™ Study provides a complementary perspective by examining how care is experienced and evaluated by those who use and purchase it. By integrating the perspectives of patients, healthcare leaders, and buyers, the study provides a more complete view of the factors that influence trust, decision-making, and long-term engagement in cross-border care.
One of its most important findings is that growth in cross-border care is not primarily constrained by demand, but by trust. Patients are willing to travel for care, but their decisions are shaped by their confidence in how that care will be coordinated, communicated, and supported throughout the journey.
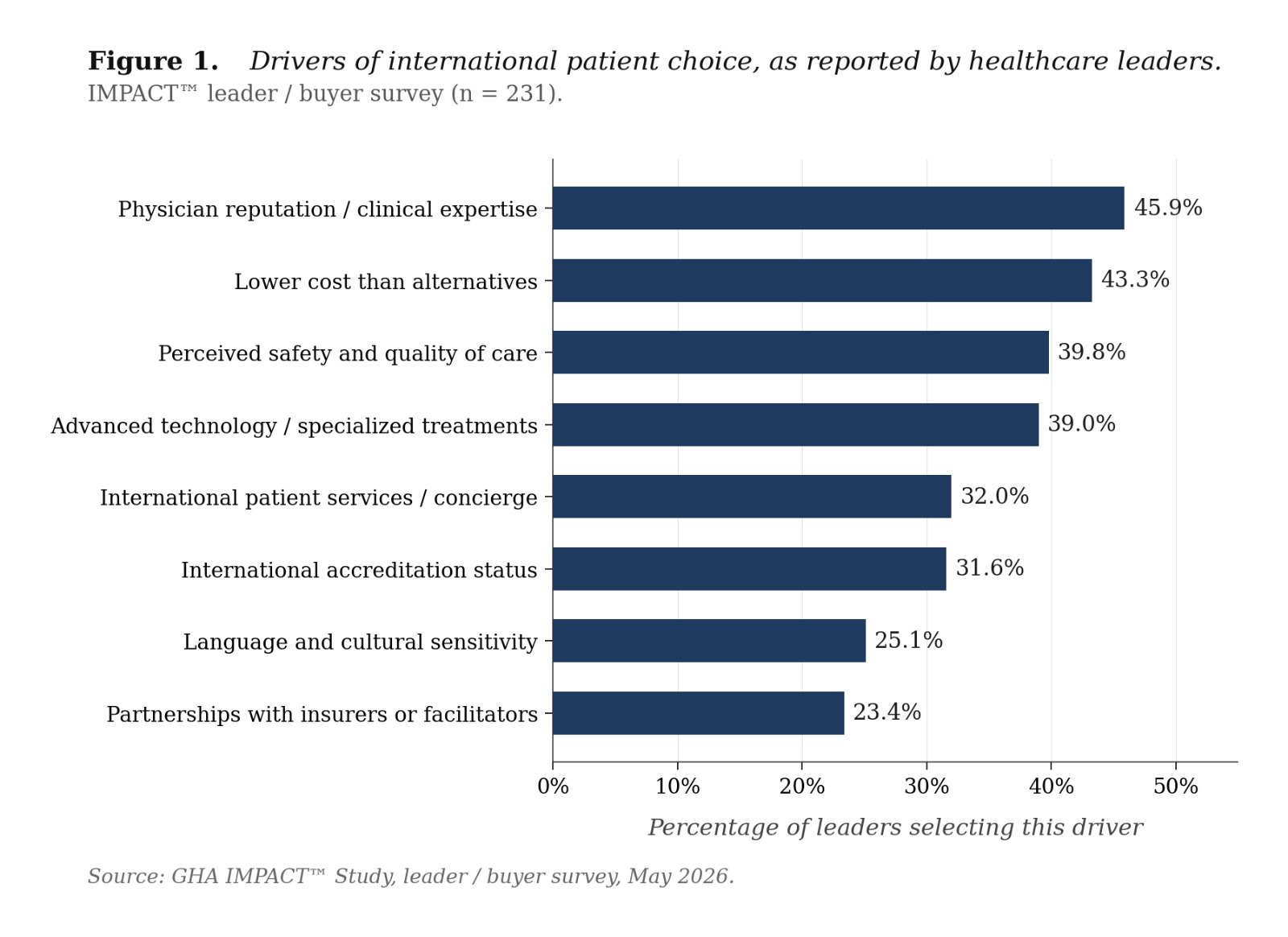
The study also highlights a gap that has direct relevance for accreditation. A significant proportion of patients receive care at accredited facilities, yet many are unaware of that accreditation status. As illustrated in the IMPACT™ analysis of patient experience by accreditation awareness, patients who recognize that a provider is accredited report higher confidence in safety, stronger satisfaction, and greater likelihood to recommend or return.
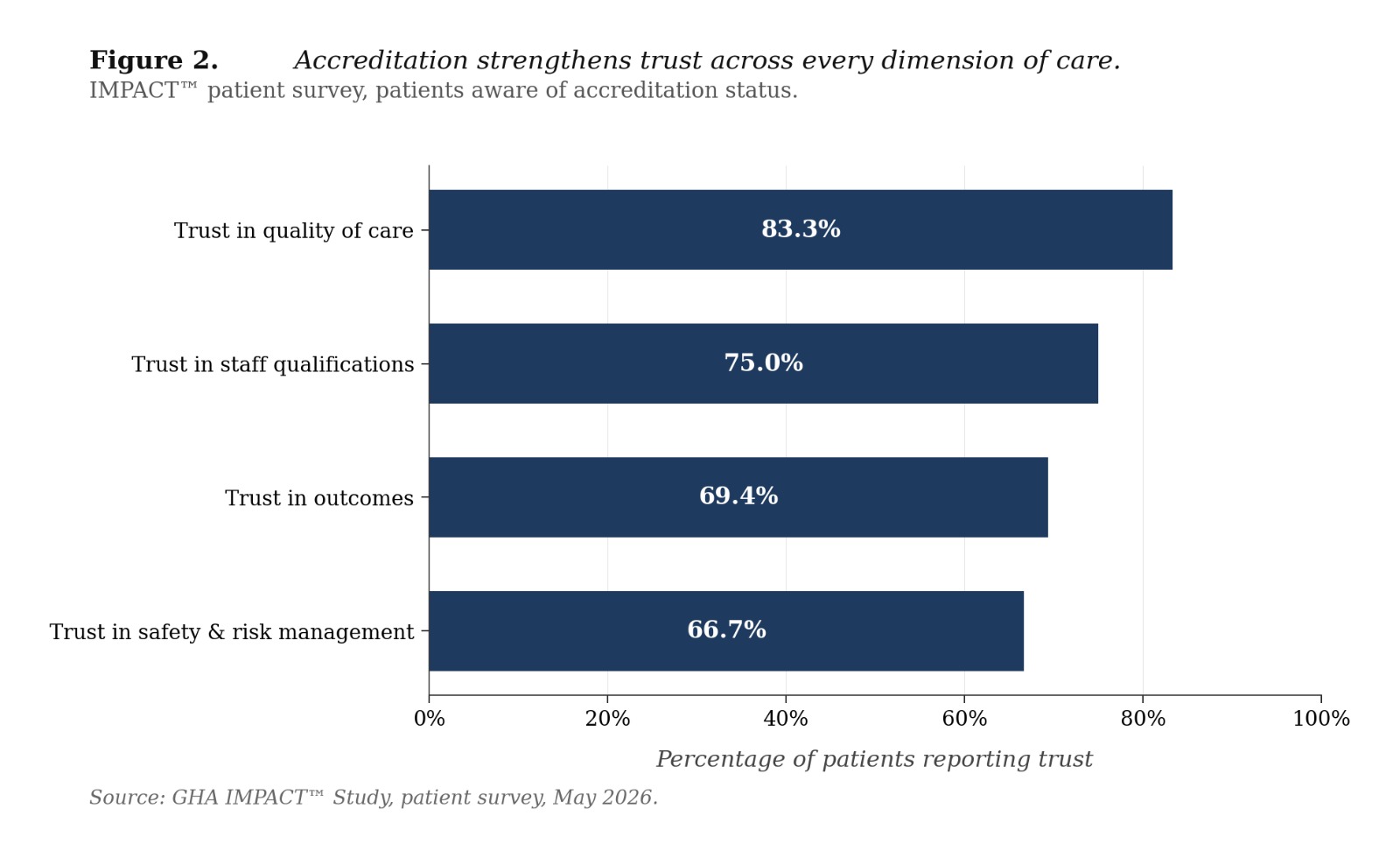
This finding reframes the role of accreditation. It is not enough to validate quality. That quality must be visible, understood, and reinforced throughout the patient journey. Accreditation, in this sense, becomes part of how trust is actively built, not simply how quality is verified.
From Experience to Systems: Where Variation Occurs
Taken together, the findings from benchmarking and IMPACT™ point toward a common conclusion. Variation in patient experience is rarely driven by the quality of clinical care alone. It is more often a reflection of how systems are designed and how responsibilities are defined across the patient journey.
Patients consistently report challenges related to communication, coordination, and follow-up, even in organizations with strong clinical reputations. These issues are not isolated events. They are patterns that emerge when processes are fragmented or when ownership is unclear.
.jpeg)
This has led to an important reframing. Patient experience is not an outcome of individual interactions. It is the result of how effectively the system functions as a whole.
This system’s perspective also clarifies why international patient services matter beyond the individuals who use them. The infrastructure that supports a coordinated cross-border journey, including governance, digital continuity, care coordination, and follow-up protocols, is the same infrastructure that strengthens domestic care for the broader population. Programs that build these capabilities for international patients consistently report downstream improvements in domestic patient experience, readmission rates, and staff retention. International patient services function as a stress test for the entire delivery system.
Implications for the Next Generation of Standards
The evolution of Accreditation 6.0 reflects a consistent finding across both benchmarking and IMPACT™ data. There is a gap between strong clinical care and inconsistent journey delivery, and this is where trust is most often lost. Organizations are not failing to deliver quality treatment. They are struggling to deliver that quality as part of a coordinated, transparent, and patient-understood experience.
Version 6.0 addresses this directly by placing greater emphasis on system-level performance, including governance, care coordination, digital continuity, workforce capability, and the communication and visibility of safety and quality. The intent is to align accreditation more closely with how care is experienced and evaluated by patients, buyers, and partners, not only how it is documented internally.
In this way, benchmarking has evolved from a retrospective exercise into a forward-looking design tool. It informs how standards are structured and ensures that they reflect the realities of care delivery, rather than idealized models of performance.
Looking Ahead
Global healthcare is increasingly being evaluated not as a series of isolated clinical encounters, but as an interconnected experience that spans systems, providers, and time. As this shift continues, the role of accreditation will depend on its ability to reflect and reinforce that reality.
The convergence of benchmarking data and multi-stakeholder insights suggests that trust is emerging as a central organizing principle in global healthcare. Accreditation remains a key contributor to that trust, but its impact will be shaped by how well it aligns with system performance and patient expectations.
The evolution of standards, therefore, is not simply a technical exercise. It is part of a broader effort to ensure that quality frameworks remain relevant in a healthcare environment that is becoming more connected, more transparent, and more accountable to those it serves.
Trust is becoming the organizing principle of global healthcare quality. Accreditation frameworks that measure it, communicate it, and reinforce it across the patient journey will remain central to how systems are evaluated. Frameworks that do not will lose relevance as patients, payers, and policymakers raise the standard of evidence they require.
The 2026 Global Medical Travel Benchmarking Report and IMPACT™ Study findings are available for citation in institutional research, accreditation strategy, policy analysis, and peer-reviewed work. Organizations interested in the underlying dataset, the Accreditation 6.0 draft standards, or collaborative benchmarking are encouraged to contact GHA directly.
*IMPACT™ is Global Healthcare Accreditation’s flagship research initiative measuring international medical travel through the eyes of patients, providers, and purchasers. It is the most comprehensive, globally benchmarked study of satisfaction, safety, trust, outcomes, and care experience in cross-border healthcare.



.png)
